SEMMELWEIS UNIVERSITY DOCTORAL SCHOOL. Correlations of tumors of the oral cavity and diabetes mellitus
|
|
|
- Balázs Kelemen
- 5 évvel ezelőtt
- Látták:
Átírás
1 SEMMELWEIS UNIVERSITY DOCTORAL SCHOOL Oncological Research Programme Correlations of tumors of the oral cavity and diabetes mellitus PhD Thesis Dr. Márta Ujpál Supervisor: Dr. Zsuzsanna Suba Programme director: Dr. András Jeney Budapest 2004.
2 Summary The oral signs of diabetes mellitus are well known: gingivitis, parodontosis, and lesions of the oral mucosa (glossitis and candiasis). However, the literature to date does not detail any connection between diabetes mellitus and tumors in the oral cavity. The author has carried out epidemiological, clinical and histopathological studies on this topic. The stomato-oncological screening of diabetics revealed that subjects with diabetes (and particularly that of type 2.) display an elevated incidence of inflammatory lesions, benign tissue growth and precancerous states. Diabetics who smoke are at high risk of the development of precancerous processes in the oral cavity. A retrospective investigation of malignant tumors in the oral cavity demonstrated an enhanced frequency of diabetics (mainly of type 2.) among thos with oral carcinoma. The most frequent malignomas among diabetics are tumors of the gingiva and the lip. It emerged from the clinical and histopathological studies that the progression of oral carcinomas is accelerated by diabetes: the tumors then form metastases more quickly, and death occurs earlier. A new hypo thesis is proposed as regards the correlation of tumors in the oral cavity and diabetes mellitus, study of which demands further detailed research work.
3 Aims The research work was aimed at answering the following questions: 1. Can an epidemiological connection be found between diabetes mellitus and tumors of the oral cavity? a. What are the incidences of oral precancerosis and tumors of the oral cavity in diabetics? b. What is the incidence of diabetes among patients with malignant tumors of the oral cavity? 2. Is there a connection between the localization of malignant tumors of the oral cavity and the symptoms/complications of diabetes mellitus? 3. Does diabetes mellitus influence the progression of oral carcinomas?
4 Materials and methods 1. Epidemiological studies The occurrence of precancerosis and tumors of the oral cavity among patients with diabetes mellitus Between 1. March and 31. January stomato-oncological screening examinations were performed on 200 diabetic patients at the 1 st and 2 nd Departments of Medicine at Semmelweis University. Of these 200 patients, 82 had diabetes of type 1, and 118 had diabetes of type 2, 131 were females, and 69 were males. The average age overall was 458 years; in the type 1 group it was 55.3 years. 2. Clinical studies 1.1. The incidence of diabetes mellitus among patients with malignant tumors of the oral cavity A retrospective sutdy was carried out on patients with histologically confirmed malignant tumors of the oral cavity who were treated at the Department of Oral and Maxillofacial Surgery at Semmelweis University between 1. January 1998 and 30. June Of the 610 patients studied, 435 were males, and 175 were females. 606 had histologically confirmed planocellular carcinoma, and 4 had adenocarcinoma. The average age of the patientswas 56 years. The control group consisted of 5-74 adults who were tumorfree, who underwent dental surgical care; their average age was 51 years. On the basis of the fasting blood sugar levels, the patients were divided into three groups: 1. a normal fasting blood sugar level (<6,1 mmol/l)., 2. an elevated fasting blood sugar level (6,1-6,9 mmol/l), i.e. an impaired fasting glucose level, indicative of a disturbance of the carbohydrate metabolism., 3. diabetes mellitus (fasting blood sugar level >6,9 mmol/l).,
5 Studies were made of the incidence of diabetes mellitus in the various tumor stages, and of the distributions of the malignomas of the oral cavity according to localization among the diabetic patients and the non-diabetic cases Study of the progression of malignant tumors of the oral cavity in diabetics Retrospective, follow-up studies were carried out on patients with histologically confirmed malignant tumors of the oral cavity, treated at the Department of Oral and Maxillofacial Surgery at Semmelweis University between 1. January 1992 and 31. December The criteria for inclusion in the study were as follows: a. a gingival tumor (The most frequent malignant tumor in diabetes mellitus)., b. tumor stage T 2-3 N 0 M 0; c. identical surgical treatment: tumor extripation + functional cervical dissection., d. no neoadjuvant treatment., e. follow-up for 2 years postoperatively. At the end of the 2-year follow-up period, a study was made of the TNM data, and hence the progression could be determined. Criteria for a diagnosis of progression: a. local recurrence., b. regional lymph node metastases., c. distant metastases., d. tumor-related death. The different types of progression were surveyed in the diabetic group and the control group, and the results were compared and analysed statistically.
6 3. Histopathological studies The surgical blocks of the patients with gingival tumors were assessed histologically from the aspect of progression in the diabetic and non-diabetic groups. The mode of invasion on the invasive front of the tumors was categorized in four grades: 1. the tumor was sharply delineated from its environment., 2. the tumor was spreading in bundles, and was not sharply delineated., 2. cell groups that had separated from the original tumor were invading the adjacent tissues., 3. the spreading was diffuse, with the invasion of tumor cells and cell groups. Immunhistochemical methods were used to evaluate the integrity of the basal membrane, and the expression of lamin-5 was studied.
7 4. Statistical methods As we were searching for a correlation between two independent variables, we used the chi-squared test for the statistical analysis, with 2 degrees of freedom. The Student twotailed t-test was employed in comparisons of histopathological samples and in studies of the differences in mean values. Significance examinations were made at a level of 5%. Statistical investigations were performed in the Department of Biophysics at Semmelweis University. Results 1. The occurrence of precancerosis and tumors of the oral cavity among patients with diabetes mellitus The lesions that were observed were classified into three groups: a. inflammatory lesions (cheilitis and glossitis)., b. benign tissue growths., c. precancerous lesions (leukoplakia and erythroplakia). Malignant lesions were not found in the 200 patients examined. Some form of lesion of the oral cavity was observed in 51.5% of the diabetic patients. In both diabetic groups, the inflammatory lesions were most frequent, followed by the benign tissue growths and then the precancerous states. The frequences of all three types of lesion were higher among the patients with diabetes of type 2 than among those with diabetes of type 1: inflammatory lesions: 31.3% and 25.6%, benign tissue growths: 16.9% and 10.9%, and precancerosis: 11% and 3.6%, respectively.
8 2. The incidence of diabetes mellitus among patients malignant tumors of the oral cavity The 610 patients with carcinoma of the oral cavity were found to include 89 diabetics (14.6%) and 59 cases (9.7%) with an elevated blood sugar level, 87 (97%) of the 89 diabetics had diabetes of type 2. The control group included 32 diabetics (5.6%) and the same number of subjects with an elevated blood sugar level. 24.3% of those with malignant tumors of the oral cavity, and 11.2% of the control group exhibited irregularities of the glucose metabolism. The difference was significant (p?0,01). There was not a significant difference in incidence if diabetes in the different tumor stages. The most frequent tumor of the oral cavity in the non-diabetic group was the sublingual carcinoma (146 cases, 28%), followed by lingual carcinoma (100 cases, 19%). Among the diabetics, the gingival tumor was most frequent (26 cases, 29%), followed ba carcinoma of the lip (21 cases, 24%). The rates of tumors of the gingiva and of the lip were significantly higher (p?0,01) among the diabetics then in the non-diabetic tumor group. 3. Study of the progression of malignant tumors of the oral cavity in diabetics 3.1. Results of clinical studies On the basis of the previously-listed criteria, 24 patients were classified into the diabetic group, and 52 into the non-diabetic group. All of the diabetics had diabetes of type 2. Among the 24 patients in the diabetic group, progression was observed in 15 cases (62.5%): 3 of the 15 progression cases involved local recurrence (20%), while the remaining 12 involved a combination of local recurrence and cervical lymph node metastases (80%). 12 of the 24 patients (50%) had died by the end of the 2-year follow-up period.
9 In the control group, 24 of the 52 cases (46%) displayed progression: 14 involved local recurrence (58%), and 10 (42%) the other form of progression. 6 of the 52 patients (11%) died. In the diabetic group, there were significantly more cases involving metastases (p?0,05) and significantly more deaths (p?0,001) during the 2-year follow-up period Histhopathological results Among the patients in the diabetic group, tumor invasion of grade 3 or 4 occured more frequently, whereas grade 1 or 2 was more characteristic in the control group. The tumor invasion was significantly more aggressive in the diabetics (p?0,01).
10 New results presented in the theis 1. Significant epidemiological correlations were found between the incidences of precancerous states and tumors of the oral cavity and the occurrence of diabetes mellitus. 2. The rates of benign tissue growths and precancerous states were higher among diabetic patients than in the general population. Precancerous processes occurred more frequently among patients with diabetes of type Diabetes of type 2 was observed significantly more often among the patients with carcinoma of the oral cavity than in the tumor-free control group (p?0,01) 4. The most frequent malignomas of the oral cavity among the diabetic patients were tumors of the gingiva and the lip, while the most common types among the nondiabetics were sublingual and lingual carcinomas. 5. Both clinically and histopathologically, the progression of the carcinomas of the oral cavity was significantly more rapid among those with diabetes mellitus of type 2 than in the non-diabetic control group (p?.0,001)
11 Publishing activity Publications connceted with the topic of thesis 1. Ujpál M., Suba Zs., Szabó Gy.: Szinkron jelentkezo melanoma malignum és gingiva carcinoma. Fogorvosi Szemle, Ujpál M., Tóth-Bagi Z.: Post mortem diagnosztizált primer multiplex daganatok 10 éves beteganyagunkban. Fogorvosi Szemle, Tóth-Bagi Z., Ujpál M.: Négy primer daganat együttes elofordulása. Fogorvosi Szemle, Ujpál M., Tóth-Bagi Z., Suba Zs., Barabás J.: Kétoldali retinoblastoma irradiatioját követo késoi leiomyosarcoma a maxillo-orbitalis régióban. Fogorvosi Szemle, Ujpál M., Barabás J., Suba Zs.: Három egymást követo elsodleges malignus tumor ritka esete a fej-nyak régióban. Orvosi Hetilap, M. Ujpál., Zs. Németh., A. Reichwein., Gy. Szabó: Long-term results following surgical treatment of benign symmetric lipomatosis (BSL) International Journal of Oral and Maxillofacial Surgery, IF: 0,972
12 7. M. Ujpál., Zs. Suba., J. Barabás., Zs. Németh., B. Szende., Gy. Szabó: Rare incidence of three consecutive primary tumors in the maxillofacial region: retinoblastoma, leiomyosarcoma, and choriocarcinoma: case report Journal Craniofacial Surgery, IF:0, Ujpál M., Matos O., Bíbok Gy., Szabó Gy.: A diabetes mellitus elofordulása malignus szájüregi daganatos betegekben Orvosi Hetilap, Zs. Németh., J. Czigner., L. Iván., M. Ujpál., J. Barabás., G. Szabó: Quadruple cancer, including tripple in the head and neck region. Report of case Neoplasma, IF: 0, Zs. Suba., Zs. Németh., M. Ujpál., Sz. Gyulai-Gaál., B. Szende., Gy. Szabó: Malignant myoepithelioma. Clinicopathological and immunohistochemical characteristics International Journal of Oral and Maxillofacial Surgery, IF: 0, Ujpál M., Matos O., Bíbok Gy., Somogyi A., Suba Zs.: Stomatoonkológiai szurovizsgálat cukorbetegek esetében Fogorvosi Szle, Zs. Németh, Gy. Dömötör, M. Tálos, J. Barabás, M. Ujpál, Gy. Szabó: Resection and replacement of the carotid artery in metastatic head and neck cancer: literature review and case report. International Journal of Oral and Maxillofacial Surgery, IF: 0,754
13 13. M. Ujpál., O. Matos., Gy. Bíbok., A. Somogyi., Gy. Szabó., Zs. Suba: Diabetes mellitus and oral tumors in Hungary. Epidemiological correlations Diabetes Care IF: 5, Ujpál M., Matos O., Bíbok Gy., Somogyi A., Szigeti K., Szabó Gy., Suba Zs.: Diabetes mellitus és szájüregi daganatok epidemiológiai összefüggései Orv. Hetilap (megjelenés alatt)
14 Publications not connected with the topics of the thesis 1. Ujpál M.: Bucaryl szövetragasztó alkalmazása az ambuláns szájsebészetben. Fogorvosi Szemle, Ujpál M., Szabó Gy. és mtsai: A benignus szimmetrikus lipomatosisról. Magyar Onkológia, Ujpál M., Szabó Gy.: A benignus szimmetrikus lipomatosis szájsebészeti vonatkozásai. Fogorvosi Szemle, , 4. Ujpál M., Szabó Gy.: A Gorlin-Goltz syndroma familiáris elofordulása. Fogorvosi Szemle, Tóth-Bagi Z., Ujpál M., Gyenes V., Tapasztalataink az Otten-féle mandibulo-maxillaris rögzítéssel. Fogorvosi Szemle, Klenk G., Ujpál M., Papp E.: A 3-dimenziós CT vizsgálatok jelentosége a szájsebészet területén. Fogorvosi Szemle, Zavaros G. Ujpál M.: Szimmetrikus exostosis az állkapcson. Fogorvosi Szemle, G. Szabó, M. Ujpál: Massive blutung aus der A. max. 11 Tage nach einer Mittelgesichtfractur. Acta Chirurgica Austriaca,
15 9. Ujpál M., Biczó Á., Huszár L., Temesvári A.-né, Tóthfalusi L., Szabó Gy.: Az Appranax és a Cataflam fájdalomcsillapító hatásának összehasonlító vizsgálata szájsebészeti beavatkozást követoen. Fogorvosi Szemle, Joób Fancsaly Á., Pataky L., Martonffy K., Ujpál M., Hrabák K.: A Gardner szindrómáról több eset kapcsán. Orvosi Hetilap, (21) Fülöp E, Ujpál M, Gyulai Gaál Sz, Bereczkei Á.: A Duomox (amoxicillin) alkalmazásának lehetoségei a szájsebészetben Dentál Hírek, Fülöp E., Ujpál M.: A szájüregi fertozések gyógyszeres kezelése Magyar Egészség Piac, Fülöp E., Ujpál M.: A szájüregi gyulladások gyógyszres kezelésének a lehetoségei Dental Hírek, Koppány F., Joób F. Á., Pataky L., Martonffy K., Ujpál M., Németh Zs., Hrabák K: Gardner-szindróma (esetismertetés) Fogorvosi Szemle,
SEMMELWEIS EGYETEM DOKTORI ISKOLA. A szájüregi daganatok és a diabetes mellitus összefüggései
 SEMMELWEIS EGYETEM DOKTORI ISKOLA Program: Onkológiai Kutatások A szájüregi daganatok és a diabetes mellitus összefüggései PhD értekezés tézisei Dr. Ujpál Márta Témavezeto: Dr. Suba Zsuzsanna egyetemi
SEMMELWEIS EGYETEM DOKTORI ISKOLA Program: Onkológiai Kutatások A szájüregi daganatok és a diabetes mellitus összefüggései PhD értekezés tézisei Dr. Ujpál Márta Témavezeto: Dr. Suba Zsuzsanna egyetemi
A rosszindulatú daganatos halálozás változása 1975 és 2001 között Magyarországon
 A rosszindulatú daganatos halálozás változása és között Eredeti közlemény Gaudi István 1,2, Kásler Miklós 2 1 MTA Számítástechnikai és Automatizálási Kutató Intézete, Budapest 2 Országos Onkológiai Intézet,
A rosszindulatú daganatos halálozás változása és között Eredeti közlemény Gaudi István 1,2, Kásler Miklós 2 1 MTA Számítástechnikai és Automatizálási Kutató Intézete, Budapest 2 Országos Onkológiai Intézet,
Gottsegen National Institute of Cardiology. Prof. A. JÁNOSI
 Myocardial Infarction Registry Pilot Study Hungarian Myocardial Infarction Register Gottsegen National Institute of Cardiology Prof. A. JÁNOSI A https://ir.kardio.hu A Web based study with quality assurance
Myocardial Infarction Registry Pilot Study Hungarian Myocardial Infarction Register Gottsegen National Institute of Cardiology Prof. A. JÁNOSI A https://ir.kardio.hu A Web based study with quality assurance
Stomato-onkológiai szûrôvizsgálatok: a korai diagnózis lehetôségei
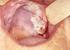 Stomato-onkológiai szûrôvizsgálatok: a korai diagnózis lehetôségei Eredeti közlemény Bánóczy Jolán 1, Bakó Attila 2, Dombi Csaba 3, Ember István 4, Kósa Zsigmond 2, Sándor János 4, Szabó György 5 1 Semmelweis
Stomato-onkológiai szûrôvizsgálatok: a korai diagnózis lehetôségei Eredeti közlemény Bánóczy Jolán 1, Bakó Attila 2, Dombi Csaba 3, Ember István 4, Kósa Zsigmond 2, Sándor János 4, Szabó György 5 1 Semmelweis
Correlation & Linear Regression in SPSS
 Petra Petrovics Correlation & Linear Regression in SPSS 4 th seminar Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Correlation
Petra Petrovics Correlation & Linear Regression in SPSS 4 th seminar Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Correlation
FAMILY STRUCTURES THROUGH THE LIFE CYCLE
 FAMILY STRUCTURES THROUGH THE LIFE CYCLE István Harcsa Judit Monostori A magyar társadalom 2012-ben: trendek és perspektívák EU összehasonlításban Budapest, 2012 november 22-23 Introduction Factors which
FAMILY STRUCTURES THROUGH THE LIFE CYCLE István Harcsa Judit Monostori A magyar társadalom 2012-ben: trendek és perspektívák EU összehasonlításban Budapest, 2012 november 22-23 Introduction Factors which
Miskolci Egyetem Gazdaságtudományi Kar Üzleti Információgazdálkodási és Módszertani Intézet. Correlation & Linear. Petra Petrovics.
 Correlation & Linear Regression in SPSS Petra Petrovics PhD Student Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Exercise
Correlation & Linear Regression in SPSS Petra Petrovics PhD Student Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Exercise
Statistical Dependence
 Statistical Dependence Petra Petrovics Statistical Dependence Deinition: Statistical dependence exists when the value o some variable is dependent upon or aected by the value o some other variable. Independent
Statistical Dependence Petra Petrovics Statistical Dependence Deinition: Statistical dependence exists when the value o some variable is dependent upon or aected by the value o some other variable. Independent
Miskolci Egyetem Gazdaságtudományi Kar Üzleti Információgazdálkodási és Módszertani Intézet Factor Analysis
 Factor Analysis Factor analysis is a multiple statistical method, which analyzes the correlation relation between data, and it is for data reduction, dimension reduction and to explore the structure. Aim
Factor Analysis Factor analysis is a multiple statistical method, which analyzes the correlation relation between data, and it is for data reduction, dimension reduction and to explore the structure. Aim
Correlation & Linear Regression in SPSS
 Correlation & Linear Regression in SPSS Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Exercise 1 - Correlation File / Open
Correlation & Linear Regression in SPSS Types of dependence association between two nominal data mixed between a nominal and a ratio data correlation among ratio data Exercise 1 - Correlation File / Open
OROSZ MÁRTA DR., GÁLFFY GABRIELLA DR., KOVÁCS DOROTTYA ÁGH TAMÁS DR., MÉSZÁROS ÁGNES DR.
 ALL RIGHTS RESERVED SOKSZOROSÍTÁSI CSAK A MTT ÉS A KIADÓ ENGEDÉLYÉVEL Az asthmás és COPD-s betegek életminõségét befolyásoló tényezõk OROSZ MÁRTA DR., GÁLFFY GABRIELLA DR., KOVÁCS DOROTTYA Semmelweis Egyetem
ALL RIGHTS RESERVED SOKSZOROSÍTÁSI CSAK A MTT ÉS A KIADÓ ENGEDÉLYÉVEL Az asthmás és COPD-s betegek életminõségét befolyásoló tényezõk OROSZ MÁRTA DR., GÁLFFY GABRIELLA DR., KOVÁCS DOROTTYA Semmelweis Egyetem
STUDENT LOGBOOK. 1 week general practice course for the 6 th year medical students SEMMELWEIS EGYETEM. Name of the student:
 STUDENT LOGBOOK 1 week general practice course for the 6 th year medical students Name of the student: Dates of the practice course: Name of the tutor: Address of the family practice: Tel: Please read
STUDENT LOGBOOK 1 week general practice course for the 6 th year medical students Name of the student: Dates of the practice course: Name of the tutor: Address of the family practice: Tel: Please read
Ultrasound biomicroscopy as a diagnostic method of corneal degeneration and inflammation
 Ultrasound biomicroscopy as a diagnostic method of corneal degeneration and inflammation Ph.D. Thesis Ákos Skribek M.D. Department of Ophthalmology Faculty of Medicine University of Szeged Szeged, Hungary
Ultrasound biomicroscopy as a diagnostic method of corneal degeneration and inflammation Ph.D. Thesis Ákos Skribek M.D. Department of Ophthalmology Faculty of Medicine University of Szeged Szeged, Hungary
A jövedelem alakulásának vizsgálata az észak-alföldi régióban az 1997-99. évi adatok alapján
 A jövedelem alakulásának vizsgálata az észak-alföldi régióban az 1997-99. évi adatok alapján Rózsa Attila Debreceni Egyetem Agrártudományi Centrum, Agrárgazdasági és Vidékfejlesztési Intézet, Számviteli
A jövedelem alakulásának vizsgálata az észak-alföldi régióban az 1997-99. évi adatok alapján Rózsa Attila Debreceni Egyetem Agrártudományi Centrum, Agrárgazdasági és Vidékfejlesztési Intézet, Számviteli
Dr Csőszi Tibor Hetenyi G. Kórház, Onkológiai Központ
 Dr Csőszi Tibor Hetenyi G. Kórház, Onkológiai Központ Azért, mert a kemoterápia bizonyított módon fokozza a gyógyulás esélyét! A kemoterápiának az a célja, hogy az esetleg, vagy biztosan visszamaradt daganatsejtek
Dr Csőszi Tibor Hetenyi G. Kórház, Onkológiai Központ Azért, mert a kemoterápia bizonyított módon fokozza a gyógyulás esélyét! A kemoterápiának az a célja, hogy az esetleg, vagy biztosan visszamaradt daganatsejtek
Miskolci Egyetem Gazdaságtudományi Kar Üzleti Információgazdálkodási és Módszertani Intézet Nonparametric Tests
 Nonparametric Tests Petra Petrovics Hypothesis Testing Parametric Tests Mean of a population Population proportion Population Standard Deviation Nonparametric Tests Test for Independence Analysis of Variance
Nonparametric Tests Petra Petrovics Hypothesis Testing Parametric Tests Mean of a population Population proportion Population Standard Deviation Nonparametric Tests Test for Independence Analysis of Variance
Mark Auspitz, Fayez Quereshy, Allan Okrainec, Alvina Tse, Sanjeev Sockalingam, Michelle Cleghorn, Timothy Jackson
 Mark Auspitz, Fayez Quereshy, Allan Okrainec, Alvina Tse, Sanjeev Sockalingam, Michelle Cleghorn, Timothy Jackson Division of General Surgery, University Health Network, University of Toronto, Toronto,
Mark Auspitz, Fayez Quereshy, Allan Okrainec, Alvina Tse, Sanjeev Sockalingam, Michelle Cleghorn, Timothy Jackson Division of General Surgery, University Health Network, University of Toronto, Toronto,
UNIVERSITY OF PUBLIC SERVICE Doctoral School of Military Sciences. AUTHOR S SUMMARY (Thesis) Balázs Laufer
 DOI azonosító: 10.17625/NKE.2013.021 UNIVERSITY OF PUBLIC SERVICE Doctoral School of Military Sciences AUTHOR S SUMMARY (Thesis) Balázs Laufer LAW ENFORCEMENT AND NATIONAL SECURITY CHALLENGES POSED BY
DOI azonosító: 10.17625/NKE.2013.021 UNIVERSITY OF PUBLIC SERVICE Doctoral School of Military Sciences AUTHOR S SUMMARY (Thesis) Balázs Laufer LAW ENFORCEMENT AND NATIONAL SECURITY CHALLENGES POSED BY
FORGÁCS ANNA 1 LISÁNYI ENDRÉNÉ BEKE JUDIT 2
 FORGÁCS ANNA 1 LISÁNYI ENDRÉNÉ BEKE JUDIT 2 Hátrányos-e az új tagállamok számára a KAP támogatások disztribúciója? Can the CAP fund distribution system be considered unfair to the new Member States? A
FORGÁCS ANNA 1 LISÁNYI ENDRÉNÉ BEKE JUDIT 2 Hátrányos-e az új tagállamok számára a KAP támogatások disztribúciója? Can the CAP fund distribution system be considered unfair to the new Member States? A
Szükségletre korrigált egészségügyi ellátás igénybevételének egyenlôtlenségei Magyarországon
 Szükségletre korrigált egészségügyi ellátás igénybevételének egyenlôtlenségei Magyarországon VITRAI József, BAKACS Márta, KAPOSVÁRI Csilla, NÉMETH Renáta BEVEZETÉS Az egészségügyi ellátás szükségletre
Szükségletre korrigált egészségügyi ellátás igénybevételének egyenlôtlenségei Magyarországon VITRAI József, BAKACS Márta, KAPOSVÁRI Csilla, NÉMETH Renáta BEVEZETÉS Az egészségügyi ellátás szükségletre
A cukorbetegség közvetlen egészségügyi költségei Magyarországon
 LAM-TUDOMÁNY EREDETI KÖZLEMÉNY A cukorbetegség közvetlen egészségügyi költségei Magyarországon VOKÓ Zoltán, NAGYJÁNOSI László, KALÓ Zoltán BEVEZETÉS A cukorbetegség jelentôs betegségterhet jelent világszerte
LAM-TUDOMÁNY EREDETI KÖZLEMÉNY A cukorbetegség közvetlen egészségügyi költségei Magyarországon VOKÓ Zoltán, NAGYJÁNOSI László, KALÓ Zoltán BEVEZETÉS A cukorbetegség jelentôs betegségterhet jelent világszerte
A magyar racka juh tejének beltartalmi változása a laktáció alatt
 A magyar racka juh tejének beltartalmi változása a laktáció alatt Nagy László Komlósi István Debreceni Egyetem Agrártudományi Centrum, Mezőgazdaságtudományi Kar, Állattenyésztés- és Takarmányozástani Tanszék,
A magyar racka juh tejének beltartalmi változása a laktáció alatt Nagy László Komlósi István Debreceni Egyetem Agrártudományi Centrum, Mezőgazdaságtudományi Kar, Állattenyésztés- és Takarmányozástani Tanszék,
Védősisak viselés és a kerékpáros fejsérülések összefüggése gyermekkorban
 A Pécsi Tudományegyetem Gyermekklinika, Sebészeti Osztály, Pécs 1 és az LKH Gyermekklinika, Sebészeti Osztály, Graz 2 közleménye Védősisak viselés és a kerékpáros fejsérülések összefüggése gyermekkorban
A Pécsi Tudományegyetem Gyermekklinika, Sebészeti Osztály, Pécs 1 és az LKH Gyermekklinika, Sebészeti Osztály, Graz 2 közleménye Védősisak viselés és a kerékpáros fejsérülések összefüggése gyermekkorban
Effect of sowing technology on the yield and harvest grain moisture content of maize (Zea mays L.) hybrids with different genotypes
 A - MurányiE:Layout 1 2/18/16 9:34 AM Page 1 Effect of sowing technology on the yield and harvest grain moisture content of maize (Zea mays L.) hybrids with different genotypes Eszter Murányi University
A - MurányiE:Layout 1 2/18/16 9:34 AM Page 1 Effect of sowing technology on the yield and harvest grain moisture content of maize (Zea mays L.) hybrids with different genotypes Eszter Murányi University
SURGICAL MANAGEMENT OF ODONTOGENIC CYSTS. SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST
 SURGICAL MANAGEMENT OF ODONTOGENIC CYSTS SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing fluid or
SURGICAL MANAGEMENT OF ODONTOGENIC CYSTS SE Arc-Állcsont-Szájsebészeti és Fogászati Klinika BUDAPEST DEFINITION A cyst is a sac with walls of connective tissue, lined by epithelium, containing fluid or
Fiatal férfi beteg sikeres kombinált neurointervenciós idegsebészeti-sugársebészet
 A carotisarteria szűkületének javasolt ellátási módját alapvetően befolyásolja, ha a szűkület mindkét oldalon szignifikáns mértékű, ha a szűkület oka előzetes nyaki besugárzás, illetve ha a betegnek intracranialis
A carotisarteria szűkületének javasolt ellátási módját alapvetően befolyásolja, ha a szűkület mindkét oldalon szignifikáns mértékű, ha a szűkület oka előzetes nyaki besugárzás, illetve ha a betegnek intracranialis
A veserákok gradálása; A veserák altípusok megoszlása Magyarországon
 A veserákok gradálása; A veserák altípusok megoszlása Magyarországon Am J Surg Pathol. 98 Oct;6(7):655-6. Prognostic significance of morphologic parameters in renal cell carcinoma. Ahogy kezdődött FuhrmanSA,LaskyLC,LimasC.
A veserákok gradálása; A veserák altípusok megoszlása Magyarországon Am J Surg Pathol. 98 Oct;6(7):655-6. Prognostic significance of morphologic parameters in renal cell carcinoma. Ahogy kezdődött FuhrmanSA,LaskyLC,LimasC.
Mapping Sequencing Reads to a Reference Genome
 Mapping Sequencing Reads to a Reference Genome High Throughput Sequencing RN Example applications: Sequencing a genome (DN) Sequencing a transcriptome and gene expression studies (RN) ChIP (chromatin immunoprecipitation)
Mapping Sequencing Reads to a Reference Genome High Throughput Sequencing RN Example applications: Sequencing a genome (DN) Sequencing a transcriptome and gene expression studies (RN) ChIP (chromatin immunoprecipitation)
Which letter(s) show(s) a. Melyik betű(k) mutat(nak) . 1 flexor muscle group? flexor izomcsoportot? . 2 extensor muscle group?
 Melyik betű(k) mutat(nak)... 1 flexor izomcsoportot?... 2 extensor izomcsoportot? Which letter(s) show(s) a. 1 flexor muscle group?. 2 extensor muscle group? A B C D 3 Nevezze meg azokat a nyálmirigyeket,
Melyik betű(k) mutat(nak)... 1 flexor izomcsoportot?... 2 extensor izomcsoportot? Which letter(s) show(s) a. 1 flexor muscle group?. 2 extensor muscle group? A B C D 3 Nevezze meg azokat a nyálmirigyeket,
EGÉSZSÉGTUDOMÁNY, LVII. ÉVFOLYAM, 2013. 4. SZÁM 2013/4
 Part II: Seasonal variations in human infections with Puumula hantavirus in Styria II. rész: Évszakos változások a Puumula hantavirus okozta humán fertőzésekben Stájerországban PROF. SIXL WOLF DIETER,
Part II: Seasonal variations in human infections with Puumula hantavirus in Styria II. rész: Évszakos változások a Puumula hantavirus okozta humán fertőzésekben Stájerországban PROF. SIXL WOLF DIETER,
A prosztata rosszindulatú daganata (BNO-10: C61) miatti mortalitás és morbiditás területi megoszlása Magyarországon
 A prosztata rosszindulatú daganata (BNO-10: C61) miatti mortalitás és morbiditás területi megoszlása Magyarországon Eredeti közlemény Siller György 1, Páldy Anna 2, Nádor Gizella 2, Vincze István 2, Zsámbokiné
A prosztata rosszindulatú daganata (BNO-10: C61) miatti mortalitás és morbiditás területi megoszlása Magyarországon Eredeti közlemény Siller György 1, Páldy Anna 2, Nádor Gizella 2, Vincze István 2, Zsámbokiné
Csípôízületi totál endoprotézis-beültetés lehetôségei csípôkörüli osteotomiát követôen
 A Pécsi Orvostudományi Egyetem Ortopédiai Klinika közleménye Csípôízületi totál endoprotézis-beültetés lehetôségei csípôkörüli osteotomiát követôen DR. BELLYEI ÁRPÁD, DR. THAN PÉTER. DR. VERMES CSABA Érkezett:
A Pécsi Orvostudományi Egyetem Ortopédiai Klinika közleménye Csípôízületi totál endoprotézis-beültetés lehetôségei csípôkörüli osteotomiát követôen DR. BELLYEI ÁRPÁD, DR. THAN PÉTER. DR. VERMES CSABA Érkezett:
Dr. Sasvári Péter Egyetemi docens
 A KKV-k Informatikai Infrastruktúrájának vizsgálata a Visegrádi országokban The Analysis Of The IT Infrastructure Among SMEs In The Visegrád Group Of Countries Dr. Sasvári Péter Egyetemi docens MultiScience
A KKV-k Informatikai Infrastruktúrájának vizsgálata a Visegrádi országokban The Analysis Of The IT Infrastructure Among SMEs In The Visegrád Group Of Countries Dr. Sasvári Péter Egyetemi docens MultiScience
novakpeter77@yahoo.com
 Ö N É L E T R A J Z SZEMÉLYES ADATOK Név DR. NOVÁK PÉTER Telefon +36-62-34-25-22 Fax +36-62-54-52-82 E-mail Állampolgárság novakpeter77@yahoo.com MAGYAR TANULMÁNYOK Dátum 1997-2004 Dátum 2004 - Szegedi
Ö N É L E T R A J Z SZEMÉLYES ADATOK Név DR. NOVÁK PÉTER Telefon +36-62-34-25-22 Fax +36-62-54-52-82 E-mail Állampolgárság novakpeter77@yahoo.com MAGYAR TANULMÁNYOK Dátum 1997-2004 Dátum 2004 - Szegedi
ACTA AGRONOMICA ÓVÁRIENSIS
 ACTA AGRONOMICA ÓVÁRIENSIS VOLUME 50. NUMBER 2. Mosonmagyaróvár 2008 2 UNIVERSITY OF WEST HUNGARY Faculty of Agricultural and Food Sciences Mosonmagyaróvár Hungary NYUGAT-MAGYARORSZÁGI EGYETEM Mezôgazdaság-
ACTA AGRONOMICA ÓVÁRIENSIS VOLUME 50. NUMBER 2. Mosonmagyaróvár 2008 2 UNIVERSITY OF WEST HUNGARY Faculty of Agricultural and Food Sciences Mosonmagyaróvár Hungary NYUGAT-MAGYARORSZÁGI EGYETEM Mezôgazdaság-
36% more maize was produced (Preliminary production data of main crops, 2014)
 Release date: 22 January 2015 Next release: 26 January 2015. Vital events, January November 2014 Number 13 36% more maize was produced (Preliminary data of main crops, 2014) In 2014 the of all major crops
Release date: 22 January 2015 Next release: 26 January 2015. Vital events, January November 2014 Number 13 36% more maize was produced (Preliminary data of main crops, 2014) In 2014 the of all major crops
PROSPECTIVE ASSESSMENT OF THE RISK OF BACTEREMIA IN CIRRHOTIC PATIENTS AFTER EUS WITH AND WITHOUT FNA
 PROSPECTIVE ASSESSMENT OF THE RISK OF BACTEREMIA IN CIRRHOTIC PATIENTS AFTER EUS WITH AND WITHOUT FNA Fernández ndez-esparrach G, Gimeno-Garc García a AZ, Pellisé M, Almela M*, Sendino O, Zabalza M, Llach
PROSPECTIVE ASSESSMENT OF THE RISK OF BACTEREMIA IN CIRRHOTIC PATIENTS AFTER EUS WITH AND WITHOUT FNA Fernández ndez-esparrach G, Gimeno-Garc García a AZ, Pellisé M, Almela M*, Sendino O, Zabalza M, Llach
NYOMÁSOS ÖNTÉS KÖZBEN ÉBREDŐ NYOMÁSVISZONYOK MÉRÉTECHNOLÓGIAI TERVEZÉSE DEVELOPMENT OF CAVITY PRESSURE MEASUREMENT FOR HIGH PRESURE DIE CASTING
 Anyagmérnöki Tudományok, 39/1 (2016) pp. 82 86. NYOMÁSOS ÖNTÉS KÖZBEN ÉBREDŐ NYOMÁSVISZONYOK MÉRÉTECHNOLÓGIAI TERVEZÉSE DEVELOPMENT OF CAVITY PRESSURE MEASUREMENT FOR HIGH PRESURE DIE CASTING LEDNICZKY
Anyagmérnöki Tudományok, 39/1 (2016) pp. 82 86. NYOMÁSOS ÖNTÉS KÖZBEN ÉBREDŐ NYOMÁSVISZONYOK MÉRÉTECHNOLÓGIAI TERVEZÉSE DEVELOPMENT OF CAVITY PRESSURE MEASUREMENT FOR HIGH PRESURE DIE CASTING LEDNICZKY
Hibridspecifikus tápanyag-és vízhasznosítás kukoricánál csernozjom talajon
 Hibridspecifikus tápanyag-és vízhasznosítás kukoricánál csernozjom talajon Karancsi Lajos Gábor Debreceni Egyetem Agrár és Gazdálkodástudományok Centruma Mezőgazdaság-, Élelmiszertudományi és Környezetgazdálkodási
Hibridspecifikus tápanyag-és vízhasznosítás kukoricánál csernozjom talajon Karancsi Lajos Gábor Debreceni Egyetem Agrár és Gazdálkodástudományok Centruma Mezőgazdaság-, Élelmiszertudományi és Környezetgazdálkodási
Miskolci Egyetem Gazdaságtudományi Kar Üzleti Információgazdálkodási és Módszertani Intézet. Nonparametric Tests. Petra Petrovics.
 Nonparametric Tests Petra Petrovics PhD Student Hypothesis Testing Parametric Tests Mean o a population Population proportion Population Standard Deviation Nonparametric Tests Test or Independence Analysis
Nonparametric Tests Petra Petrovics PhD Student Hypothesis Testing Parametric Tests Mean o a population Population proportion Population Standard Deviation Nonparametric Tests Test or Independence Analysis
HALLGATÓI KÉRDŐÍV ÉS TESZT ÉRTÉKELÉSE
 HALLGATÓI KÉRDŐÍV ÉS TESZT ÉRTÉKELÉSE EVALUATION OF STUDENT QUESTIONNAIRE AND TEST Daragó László, Dinyáné Szabó Marianna, Sára Zoltán, Jávor András Semmelweis Egyetem, Egészségügyi Informatikai Fejlesztő
HALLGATÓI KÉRDŐÍV ÉS TESZT ÉRTÉKELÉSE EVALUATION OF STUDENT QUESTIONNAIRE AND TEST Daragó László, Dinyáné Szabó Marianna, Sára Zoltán, Jávor András Semmelweis Egyetem, Egészségügyi Informatikai Fejlesztő
Supporting Information
 Supporting Information Cell-free GFP simulations Cell-free simulations of degfp production were consistent with experimental measurements (Fig. S1). Dual emmission GFP was produced under a P70a promoter
Supporting Information Cell-free GFP simulations Cell-free simulations of degfp production were consistent with experimental measurements (Fig. S1). Dual emmission GFP was produced under a P70a promoter
EN United in diversity EN A8-0206/419. Amendment
 22.3.2019 A8-0206/419 419 Article 2 paragraph 4 point a point i (i) the identity of the road transport operator; (i) the identity of the road transport operator by means of its intra-community tax identification
22.3.2019 A8-0206/419 419 Article 2 paragraph 4 point a point i (i) the identity of the road transport operator; (i) the identity of the road transport operator by means of its intra-community tax identification
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE január/ January 2019
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
 ó Ú ő ó ó ó ö ó ó ő ö ó ö ö ő ö ó ö ö ö ö ó ó ó ó ó ö ó ó ó ó Ú ö ö ó ó Ú ú ó ó ö ó Ű ő ó ó ó ő ó ó ó ó ö ó ó ó ö ő ö ó ó ó Ú ó ó ö ó ö ó ö ő ó ó ó ó Ú ö ö ő ő ó ó ö ö ó ö ó ó ó ö ö ő ö Ú ó ó ó ü ú ú ű
ó Ú ő ó ó ó ö ó ó ő ö ó ö ö ő ö ó ö ö ö ö ó ó ó ó ó ö ó ó ó ó Ú ö ö ó ó Ú ú ó ó ö ó Ű ő ó ó ó ő ó ó ó ó ö ó ó ó ö ő ö ó ó ó Ú ó ó ö ó ö ó ö ő ó ó ó ó Ú ö ö ő ő ó ó ö ö ó ö ó ó ó ö ö ő ö Ú ó ó ó ü ú ú ű
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE november/ November 2017
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE január/ January 2017
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE december / December 2015
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
Szívkatéterek hajlékonysága, meghajlítása
 Szívkatéterek hajlékonysága, meghajlítása Összefoglalás A szívkatéter egy olyan intravaszkuláris katéter, amelyet a szívbe vezetnek, ültetnek be diagnosztikus vagy terápiás célból. A katéterek felvezetés/eltávolítás
Szívkatéterek hajlékonysága, meghajlítása Összefoglalás A szívkatéter egy olyan intravaszkuláris katéter, amelyet a szívbe vezetnek, ültetnek be diagnosztikus vagy terápiás célból. A katéterek felvezetés/eltávolítás
Cashback 2015 Deposit Promotion teljes szabályzat
 Cashback 2015 Deposit Promotion teljes szabályzat 1. Definitions 1. Definíciók: a) Account Client s trading account or any other accounts and/or registers maintained for Számla Az ügyfél kereskedési számlája
Cashback 2015 Deposit Promotion teljes szabályzat 1. Definitions 1. Definíciók: a) Account Client s trading account or any other accounts and/or registers maintained for Számla Az ügyfél kereskedési számlája
Lohe mûtét hosszú távú eredményei a metatarsalgia kezelésében
 POTE Ortopédiai Klinika közleménye Lohe mûtét hosszú távú eredményei a metatarsalgia kezelésében DR. LOVÁSZ GYÖRGY, DR. KRÁNICZ JÁNOS, DR. SCHMIDT BÉLA Érkezett: 1995. április 11. ÖSSZEFOGLALÁS A szerzôk
POTE Ortopédiai Klinika közleménye Lohe mûtét hosszú távú eredményei a metatarsalgia kezelésében DR. LOVÁSZ GYÖRGY, DR. KRÁNICZ JÁNOS, DR. SCHMIDT BÉLA Érkezett: 1995. április 11. ÖSSZEFOGLALÁS A szerzôk
Áttekintés az emlőrák megbetegedések és a gyógyítás helyzetéről Magyarországon beleértve a 2001 óta folyó mammográfiás szűréseket. Dr.
 Áttekintés az emlőrák megbetegedések és a gyógyítás helyzetéről Magyarországon beleértve a 2001 óta folyó mammográfiás szűréseket. Dr. Kovács Attila 1 Emlőrák Világszerte a 5. leggyakoribb rák nőkben (valamennyi
Áttekintés az emlőrák megbetegedések és a gyógyítás helyzetéről Magyarországon beleértve a 2001 óta folyó mammográfiás szűréseket. Dr. Kovács Attila 1 Emlőrák Világszerte a 5. leggyakoribb rák nőkben (valamennyi
fogyasztói ATTITŰDÖk Az ALmApIACon CONSUmER ATTITUDE TO APPLE
 The hungarian Journal of food, nutrition and MarkeTing FELFÖLDI János, APÁTI Ferenc, SZABÓ Viktor, NÁBRÁDI András Debreceni Egyetem, Agrár- és műszaki Tudományok Centruma, Agrárgazdasági és Vidékfejlesztési
The hungarian Journal of food, nutrition and MarkeTing FELFÖLDI János, APÁTI Ferenc, SZABÓ Viktor, NÁBRÁDI András Debreceni Egyetem, Agrár- és műszaki Tudományok Centruma, Agrárgazdasági és Vidékfejlesztési
EPILEPSY TREATMENT: VAGUS NERVE STIMULATION. Sakoun Phommavongsa November 12, 2013
 EPILEPSY TREATMENT: VAGUS NERVE STIMULATION Sakoun Phommavongsa November 12, 2013 WHAT IS EPILEPSY? A chronic neurological disorder characterized by having two or more unprovoked seizures Affects nearly
EPILEPSY TREATMENT: VAGUS NERVE STIMULATION Sakoun Phommavongsa November 12, 2013 WHAT IS EPILEPSY? A chronic neurological disorder characterized by having two or more unprovoked seizures Affects nearly
2 kultúra. Zétényi Tamás. www.nytud.hu/depts/tlp/quantification zetenyi@nytud.hu
 2 kultúra Zétényi Tamás www.nytud.hu/depts/tlp/quantification zetenyi@nytud.hu MTA Nyelvtudományi Intézet - 'Elmélet és kísérlet a nyelvészetben' Budapest, 2014. február 25 agenda: mit csinálunk? mit veszünk
2 kultúra Zétényi Tamás www.nytud.hu/depts/tlp/quantification zetenyi@nytud.hu MTA Nyelvtudományi Intézet - 'Elmélet és kísérlet a nyelvészetben' Budapest, 2014. február 25 agenda: mit csinálunk? mit veszünk
Construction of a cube given with its centre and a sideline
 Transformation of a plane of projection Construction of a cube given with its centre and a sideline Exercise. Given the center O and a sideline e of a cube, where e is a vertical line. Construct the projections
Transformation of a plane of projection Construction of a cube given with its centre and a sideline Exercise. Given the center O and a sideline e of a cube, where e is a vertical line. Construct the projections
KELET-ÁZSIAI DUPLANÁDAS HANGSZEREK ÉS A HICHIRIKI HASZNÁLATA A 20. SZÁZADI ÉS A KORTÁRS ZENÉBEN
 Liszt Ferenc Zeneművészeti Egyetem 28. számú művészet- és művelődéstörténeti tudományok besorolású doktori iskola KELET-ÁZSIAI DUPLANÁDAS HANGSZEREK ÉS A HICHIRIKI HASZNÁLATA A 20. SZÁZADI ÉS A KORTÁRS
Liszt Ferenc Zeneművészeti Egyetem 28. számú művészet- és művelődéstörténeti tudományok besorolású doktori iskola KELET-ÁZSIAI DUPLANÁDAS HANGSZEREK ÉS A HICHIRIKI HASZNÁLATA A 20. SZÁZADI ÉS A KORTÁRS
Miskolci Egyetem Gazdaságtudományi Kar Üzleti Információgazdálkodási és Módszertani Intézet. Hypothesis Testing. Petra Petrovics.
 Hypothesis Testing Petra Petrovics PhD Student Inference from the Sample to the Population Estimation Hypothesis Testing Estimation: how can we determine the value of an unknown parameter of a population
Hypothesis Testing Petra Petrovics PhD Student Inference from the Sample to the Population Estimation Hypothesis Testing Estimation: how can we determine the value of an unknown parameter of a population
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE február/ February 2019
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE június/ June 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE augusztus/ August 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE július/ July 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE október/ October 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE március/ March 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE szeptember/ September 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE december/ December 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE november/ November 2018
 AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
AZ NFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE NATIONAL EMPLOYMENT SERVICE Nyilvántartott álláskeresők összesen Registered jobseekers total Ebből / From this Kategóriák / Categories álláskeresési
 Társadalmi-gazdasági szempontok Az ipari termelési folyamatok kedvezőbbé tétele és az ipari együttműködési láncok sűrűsége pozitív társadalmi és gazdasági eredmények létrejöttéhez is hozzájárul. A társadalmi
Társadalmi-gazdasági szempontok Az ipari termelési folyamatok kedvezőbbé tétele és az ipari együttműködési láncok sűrűsége pozitív társadalmi és gazdasági eredmények létrejöttéhez is hozzájárul. A társadalmi
ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY
 ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY A feladatsor három részbol áll 1. A vizsgáztató társalgást kezdeményez a vizsgázóval. 2. A vizsgázó egy szituációs feladatban vesz részt a
ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY A feladatsor három részbol áll 1. A vizsgáztató társalgást kezdeményez a vizsgázóval. 2. A vizsgázó egy szituációs feladatban vesz részt a
USER MANUAL Guest user
 USER MANUAL Guest user 1 Welcome in Kutatótér (Researchroom) Top menu 1. Click on it and the left side menu will pop up 2. With the slider you can make left side menu visible 3. Font side: enlarging font
USER MANUAL Guest user 1 Welcome in Kutatótér (Researchroom) Top menu 1. Click on it and the left side menu will pop up 2. With the slider you can make left side menu visible 3. Font side: enlarging font
A TÓGAZDASÁGI HALTERMELÉS SZERKEZETÉNEK ELEMZÉSE. SZATHMÁRI LÁSZLÓ d r.- TENK ANTAL dr. ÖSSZEFOGLALÁS
 A TÓGAZDASÁGI HALTERMELÉS SZERKEZETÉNEK ELEMZÉSE SZATHMÁRI LÁSZLÓ d r.- TENK ANTAL dr. ÖSSZEFOGLALÁS A hazai tógazdasági haltermelés a 90-es évek közepén tapasztalt mélypontról elmozdult és az utóbbi három
A TÓGAZDASÁGI HALTERMELÉS SZERKEZETÉNEK ELEMZÉSE SZATHMÁRI LÁSZLÓ d r.- TENK ANTAL dr. ÖSSZEFOGLALÁS A hazai tógazdasági haltermelés a 90-es évek közepén tapasztalt mélypontról elmozdult és az utóbbi három
Választási modellek 3
 Választási modellek 3 Prileszky István Doktori Iskola 2018 http://www.sze.hu/~prile Forrás: A Self Instructing Course in Mode Choice Modeling: Multinomial and Nested Logit Models Prepared For U.S. Department
Választási modellek 3 Prileszky István Doktori Iskola 2018 http://www.sze.hu/~prile Forrás: A Self Instructing Course in Mode Choice Modeling: Multinomial and Nested Logit Models Prepared For U.S. Department
Publications: 4. Nagykálnai T, Landherr L, Németh GY: Recidiváló epipharynx tumorok lokális rádiumkezelése. Fül-Orr-Gégegyógyászat 31: 97-101, 1985.
 1 Publications: 1. Landherr L, Siminszky M, Patonay P, Patyánik M, Stumpf J. Bucca tumoros betegeink 3 és 5 éves túlélési eredményei 285 kezelt esetnél. MFE Szájsebészeti Szekció Kongresszusának gyűjteményes
1 Publications: 1. Landherr L, Siminszky M, Patonay P, Patyánik M, Stumpf J. Bucca tumoros betegeink 3 és 5 éves túlélési eredményei 285 kezelt esetnél. MFE Szájsebészeti Szekció Kongresszusának gyűjteményes
A HULLATÉK-ANALÍZIS ÉS A GYOMORTARTALOM ELEMZÉS ÖSSZE- HASONLÍTÁSA VÖRÖS RÓKA TÁPLÁLKOZÁS VIZSGÁLATA SORÁN
 A HULLATÉK-ANALÍZIS ÉS A GYOMORTARTALOM ELEMZÉS ÖSSZE- HASONLÍTÁSA VÖRÖS RÓKA TÁPLÁLKOZÁS VIZSGÁLATA SORÁN Szôcs Emese¹, Lanszki József², Heltai Miklós¹ és Szabó László¹ ¹Szent István Egyetem, Vadbiológiai
A HULLATÉK-ANALÍZIS ÉS A GYOMORTARTALOM ELEMZÉS ÖSSZE- HASONLÍTÁSA VÖRÖS RÓKA TÁPLÁLKOZÁS VIZSGÁLATA SORÁN Szôcs Emese¹, Lanszki József², Heltai Miklós¹ és Szabó László¹ ¹Szent István Egyetem, Vadbiológiai
Supplementary materials to: Whole-mount single molecule FISH method for zebrafish embryo
 Supplementary materials to: Whole-mount single molecule FISH method for zebrafish embryo Yuma Oka and Thomas N. Sato Supplementary Figure S1. Whole-mount smfish with and without the methanol pretreatment.
Supplementary materials to: Whole-mount single molecule FISH method for zebrafish embryo Yuma Oka and Thomas N. Sato Supplementary Figure S1. Whole-mount smfish with and without the methanol pretreatment.
Expansion of Red Deer and afforestation in Hungary
 Expansion of Red Deer and afforestation in Hungary László Szemethy, Róbert Lehoczki, Krisztián Katona, Norbert Bleier, Sándor Csányi www.vmi.szie.hu Background and importance large herbivores are overpopulated
Expansion of Red Deer and afforestation in Hungary László Szemethy, Róbert Lehoczki, Krisztián Katona, Norbert Bleier, Sándor Csányi www.vmi.szie.hu Background and importance large herbivores are overpopulated
Utolsó frissítés / Last update: február Szerkesztő / Editor: Csatlós Árpádné
 Utolsó frissítés / Last update: 2016. február Szerkesztő / Editor: Csatlós Árpádné TARTALOM / Contents BEVEZETŐ / Introduction... 2 FELNŐTT TAGBÉLYEGEK / Adult membership stamps... 3 IFJÚSÁGI TAGBÉLYEGEK
Utolsó frissítés / Last update: 2016. február Szerkesztő / Editor: Csatlós Árpádné TARTALOM / Contents BEVEZETŐ / Introduction... 2 FELNŐTT TAGBÉLYEGEK / Adult membership stamps... 3 IFJÚSÁGI TAGBÉLYEGEK
2. Local communities involved in landscape architecture in Óbuda
 Év Tájépítésze pályázat - Wallner Krisztina 2. Közösségi tervezés Óbudán Óbuda jelmondata: Közösséget építünk, ennek megfelelően a formálódó helyi közösségeket bevonva fejlesztik a közterületeket. Békásmegyer-Ófaluban
Év Tájépítésze pályázat - Wallner Krisztina 2. Közösségi tervezés Óbudán Óbuda jelmondata: Közösséget építünk, ennek megfelelően a formálódó helyi közösségeket bevonva fejlesztik a közterületeket. Békásmegyer-Ófaluban
Néhány folyóiratkereső rendszer felsorolása és példa segítségével vázlatos bemutatása Sasvári Péter
 Néhány folyóiratkereső rendszer felsorolása és példa segítségével vázlatos bemutatása Sasvári Péter DOI: http://doi.org/10.13140/rg.2.2.28994.22721 A tudományos közlemények írása minden szakma művelésének
Néhány folyóiratkereső rendszer felsorolása és példa segítségével vázlatos bemutatása Sasvári Péter DOI: http://doi.org/10.13140/rg.2.2.28994.22721 A tudományos közlemények írása minden szakma művelésének
DR. BOROMISZA ZSOMBOR. A Velencei-tóhoz kapcsolódó tájvédelmi szakértői tevékenység
 DR. BOROMISZA ZSOMBOR A Velencei-tóhoz kapcsolódó tájvédelmi szakértői tevékenység A Velencei-tavi tájhoz kapcsolódó személyes kötődésem diplomaterv, tdk dolgozat, majd doktori disszertáció formájában
DR. BOROMISZA ZSOMBOR A Velencei-tóhoz kapcsolódó tájvédelmi szakértői tevékenység A Velencei-tavi tájhoz kapcsolódó személyes kötődésem diplomaterv, tdk dolgozat, majd doktori disszertáció formájában
BKI13ATEX0030/1 EK-Típus Vizsgálati Tanúsítvány/ EC-Type Examination Certificate 1. kiegészítés / Amendment 1 MSZ EN 60079-31:2014
 (1) EK-TípusVizsgálati Tanúsítvány (2) A potenciálisan robbanásveszélyes környezetben történő alkalmazásra szánt berendezések, védelmi rendszerek 94/9/EK Direktíva / Equipment or Protective Systems Intended
(1) EK-TípusVizsgálati Tanúsítvány (2) A potenciálisan robbanásveszélyes környezetben történő alkalmazásra szánt berendezések, védelmi rendszerek 94/9/EK Direktíva / Equipment or Protective Systems Intended
Harvested production of cereals increases about one third in 2013 (Preliminary production data of main crops, 2013)
 Release date: 22 January 2014 Next release: 24 January 2014. Vital events, January November 2013 Number 13 Harvested of cereals increases about one third in 2013 (Preliminary data of main crops, 2013)
Release date: 22 January 2014 Next release: 24 January 2014. Vital events, January November 2013 Number 13 Harvested of cereals increases about one third in 2013 (Preliminary data of main crops, 2013)
A STRATÉGIAALKOTÁS FOLYAMATA
 BUDAPESTI CORVINUS EGYETEM VÁLLALATGAZDASÁGTAN INTÉZET VERSENYKÉPESSÉG KUTATÓ KÖZPONT Szabó Zsolt Roland: A STRATÉGIAALKOTÁS FOLYAMATA VERSENYBEN A VILÁGGAL 2004 2006 GAZDASÁGI VERSENYKÉPESSÉGÜNK VÁLLALATI
BUDAPESTI CORVINUS EGYETEM VÁLLALATGAZDASÁGTAN INTÉZET VERSENYKÉPESSÉG KUTATÓ KÖZPONT Szabó Zsolt Roland: A STRATÉGIAALKOTÁS FOLYAMATA VERSENYBEN A VILÁGGAL 2004 2006 GAZDASÁGI VERSENYKÉPESSÉGÜNK VÁLLALATI
Nevezze meg a jelölt csontot latinul! Name the bone marked! Nevezze meg a jelölt csont típusát! What is the type of the bone marked?
 1 Nevezze meg a jelölt csontot latinul! Name the bone marked! 2 Nevezze meg a jelölt csont típusát! What is the type of the bone marked? 3 Milyen csontállomány található a jelölt csont belsejében? What
1 Nevezze meg a jelölt csontot latinul! Name the bone marked! 2 Nevezze meg a jelölt csont típusát! What is the type of the bone marked? 3 Milyen csontállomány található a jelölt csont belsejében? What
A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2012. július
 A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2012. július A foglalkoztatók az illetékes kirendeltségeken 2012. július hónap folyamán összesen 37,9 ezer
A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2012. július A foglalkoztatók az illetékes kirendeltségeken 2012. július hónap folyamán összesen 37,9 ezer
E L İ T E R J E S Z T É S
 AZ ELİTERJESZTÉS SORSZÁMA: 201. MELLÉKLET : 1 db TÁRGY: Partnervárosi együttmőködés aláírása E L İ T E R J E S Z T É S SZEKSZÁRD MEGYEI JOGÚ VÁROS ÖNKORMÁNYZATA KÖZGYŐLÉSÉNEK 2013. június 27-i ÜLÉSÉRE
AZ ELİTERJESZTÉS SORSZÁMA: 201. MELLÉKLET : 1 db TÁRGY: Partnervárosi együttmőködés aláírása E L İ T E R J E S Z T É S SZEKSZÁRD MEGYEI JOGÚ VÁROS ÖNKORMÁNYZATA KÖZGYŐLÉSÉNEK 2013. június 27-i ÜLÉSÉRE
A tüdőrák hazai gyógyszeres kezelésének elemzése
 Eredeti közlemény 33 A tüdőrák hazai gyógyszeres kezelésének elemzése Moldvay Judit 1, Rokszin György 2, Abonyi-Tóth Zsolt 2, Katona Lajos 3, Kovács Gábor 4 1 Semmelweis Egyetem Pulmonológiai Klinika,
Eredeti közlemény 33 A tüdőrák hazai gyógyszeres kezelésének elemzése Moldvay Judit 1, Rokszin György 2, Abonyi-Tóth Zsolt 2, Katona Lajos 3, Kovács Gábor 4 1 Semmelweis Egyetem Pulmonológiai Klinika,
Animal welfare, etológia és tartástechnológia
 Animal welfare, etológia és tartástechnológia Animal welfare, ethology and housing systems Volume 4 Issue 2 Különszám Gödöllı 2008 654 EGYEDILEG ÉS KETTESÉVEL ELHELYEZETT SZOPTATÓ KOCÁK TERMELÉSI EREDMÉNYEINEK
Animal welfare, etológia és tartástechnológia Animal welfare, ethology and housing systems Volume 4 Issue 2 Különszám Gödöllı 2008 654 EGYEDILEG ÉS KETTESÉVEL ELHELYEZETT SZOPTATÓ KOCÁK TERMELÉSI EREDMÉNYEINEK
AZ ANABOLIKUS ÉS SZEKVENCIÁLIS KEZELÉS HELYE AZ OSTEOPOROSIS TERÁPIÁJÁBAN
 AZ ANABOLIKUS ÉS SZEKVENCIÁLIS KEZELÉS HELYE AZ OSTEOPOROSIS TERÁPIÁJÁBAN SEMMELWEIS EGYETEM Általános Orvostudományi Kar Semmelweis Egyetem Anabolikus kezelések teriparatid abaloparatid romosozumab Szekvenciális
AZ ANABOLIKUS ÉS SZEKVENCIÁLIS KEZELÉS HELYE AZ OSTEOPOROSIS TERÁPIÁJÁBAN SEMMELWEIS EGYETEM Általános Orvostudományi Kar Semmelweis Egyetem Anabolikus kezelések teriparatid abaloparatid romosozumab Szekvenciális
First experiences with Gd fuel assemblies in. Tamás Parkó, Botond Beliczai AER Symposium 2009.09.21 25.
 First experiences with Gd fuel assemblies in the Paks NPP Tams Parkó, Botond Beliczai AER Symposium 2009.09.21 25. Introduction From 2006 we increased the heat power of our units by 8% For reaching this
First experiences with Gd fuel assemblies in the Paks NPP Tams Parkó, Botond Beliczai AER Symposium 2009.09.21 25. Introduction From 2006 we increased the heat power of our units by 8% For reaching this
KORRÓZIÓS FIGYELÕ korrózióvédelmi mûszaki tudományos folyóirat. Szerkeszti: a szerkesztõbizottság. A szerkesztõbizottság elnöke: Zanathy Valéria
 LIII. évfolyam 3. szám 2013 KORRÓZIÓS FIGYELÕ korrózióvédelmi mûszaki tudományos folyóirat Szerkeszti: a szerkesztõbizottság A szerkesztõbizottság elnöke: Zanathy Valéria Dalmay Gábor Dr. Haskó Ferenc
LIII. évfolyam 3. szám 2013 KORRÓZIÓS FIGYELÕ korrózióvédelmi mûszaki tudományos folyóirat Szerkeszti: a szerkesztõbizottság A szerkesztõbizottság elnöke: Zanathy Valéria Dalmay Gábor Dr. Haskó Ferenc
Statistical Inference
 Petra Petrovics Statistical Inference 1 st lecture Descriptive Statistics Inferential - it is concerned only with collecting and describing data Population - it is used when tentative conclusions about
Petra Petrovics Statistical Inference 1 st lecture Descriptive Statistics Inferential - it is concerned only with collecting and describing data Population - it is used when tentative conclusions about
Márkaépítés a YouTube-on
 Márkaépítés a YouTube-on Tv+ Adj hozzá YouTube-ot, Google Ground, 2016 Március 7. Bíró Pál, Google - YouTube 9,000,000 INTERNETTEL BÍRÓ ESZKÖZÖK VOLUMENE GLOBÁLISAN WEARABLES OKOS TV 8,000,000 7,000,000
Márkaépítés a YouTube-on Tv+ Adj hozzá YouTube-ot, Google Ground, 2016 Március 7. Bíró Pál, Google - YouTube 9,000,000 INTERNETTEL BÍRÓ ESZKÖZÖK VOLUMENE GLOBÁLISAN WEARABLES OKOS TV 8,000,000 7,000,000
OncotypeDX az emlőrák kezelésében
 OncotypeDX az emlőrák kezelésében Dr. Nagy Zoltán Med Gen-Sol Kft. Szenológiai Kongresszus Kecskemét 2018. 04. 13-14. Slide 1 Az Oncotype DX korai emlőrák teszt 16 tumorral kapcsolatos gén Ösztrogén csoprt
OncotypeDX az emlőrák kezelésében Dr. Nagy Zoltán Med Gen-Sol Kft. Szenológiai Kongresszus Kecskemét 2018. 04. 13-14. Slide 1 Az Oncotype DX korai emlőrák teszt 16 tumorral kapcsolatos gén Ösztrogén csoprt
AZ ÁFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE HUNGARIAN PUBLIC EMPLOYMENT SERVICE október / October 2008
 AZ ÁFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE HUNGARIAN PUBLIC EMPLOYMENT SERVICE Kategóriák / Categories Létszám, fő Number of képest / Changes compared to previous Változás az előző
AZ ÁFSZ ADATAINAK ÖSSZEFOGLALÓ TÁBLÁZATA SUMMARY REPORT OF THE HUNGARIAN PUBLIC EMPLOYMENT SERVICE Kategóriák / Categories Létszám, fő Number of képest / Changes compared to previous Változás az előző
PUBLIKÁCIÓK JEGYZÉKE FOLYÓIRATBAN MEGJELENT IN EXTENSO KÖZLEMÉNY
 PUBLIKÁCIÓK JEGYZÉKE FOLYÓIRATBAN MEGJELENT IN EXTENSO KÖZLEMÉNY 1. Maráz K., Gorzó I., Olasz T., Kapros P.: Szövődményes periapicalis elváltozás konzervatív kezelése. Egy eset kapcsán a kalcium-hidroxidról.
PUBLIKÁCIÓK JEGYZÉKE FOLYÓIRATBAN MEGJELENT IN EXTENSO KÖZLEMÉNY 1. Maráz K., Gorzó I., Olasz T., Kapros P.: Szövődményes periapicalis elváltozás konzervatív kezelése. Egy eset kapcsán a kalcium-hidroxidról.
Phenotype. Genotype. It is like any other experiment! What is a bioinformatics experiment? Remember the Goal. Infectious Disease Paradigm
 It is like any other experiment! What is a bioinformatics experiment? You need to know your data/input sources You need to understand your methods and their assumptions You need a plan to get from point
It is like any other experiment! What is a bioinformatics experiment? You need to know your data/input sources You need to understand your methods and their assumptions You need a plan to get from point
ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY
 ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY A feladatsor három részből áll 1. A vizsgáztató társalgást kezdeményez a vizsgázóval. 2. A vizsgázó egy szituációs feladatban vesz részt a
ANGOL NYELV KÖZÉPSZINT SZÓBELI VIZSGA I. VIZSGÁZTATÓI PÉLDÁNY A feladatsor három részből áll 1. A vizsgáztató társalgást kezdeményez a vizsgázóval. 2. A vizsgázó egy szituációs feladatban vesz részt a
A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2013. január
 A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2013. január A támogatott munkaerıigények domináltak januárban Az év elsı hónapjában több mint három ezer
A munkaerı-piaci helyzet alakulása a Nemzeti Foglalkoztatási Szolgálat legfrissebb adatai alapján 2013. január A támogatott munkaerıigények domináltak januárban Az év elsı hónapjában több mint három ezer
Utolsó frissítés / Last update: Szeptember / September Szerkesztő / Editor: Csatlós Árpádné
 Utolsó frissítés / Last update: 2018. Szeptember / September Szerkesztő / Editor: Csatlós Árpádné TARTALOM / Contents BEVEZETŐ / Introduction... 2 FELNŐTT TAGBÉLYEGEK / Adult membership stamps... 3 IFJÚSÁGI
Utolsó frissítés / Last update: 2018. Szeptember / September Szerkesztő / Editor: Csatlós Árpádné TARTALOM / Contents BEVEZETŐ / Introduction... 2 FELNŐTT TAGBÉLYEGEK / Adult membership stamps... 3 IFJÚSÁGI
